Health
Why Anxiety Relief Plays a Critical Role in Pelvic Floor Muscle Relaxation
Persistent pelvic tension often feels mysterious to people experiencing it. A sense of tightness, pressure, discomfort during sitting, or pain during intimate activity may appear without a clear physical injury. Many individuals search for structural explanations such as muscle strain or posture imbalance. The deeper driver frequently lies in the nervous system rather than the muscle tissue itself.
Anxiety places the body into a protective state that prepares muscles for perceived danger. Muscles across the body subtly tighten, including those deep inside the pelvis. Over time, repeated stress responses condition the pelvic floor to remain contracted even during rest. This state contributes to what clinicians describe as a Hypertonic Pelvic Floor a condition where muscles remain shortened and unable to fully relax.
Calming anxiety interrupts that neurological loop. When the brain perceives safety, the autonomic nervous system shifts toward a restorative mode. Muscles soften, breathing deepens, and circulation improves throughout the pelvis. This change directly influences pelvic floor tone and can gradually reduce symptoms that once seemed purely physical.
The Neurological Connection Between Anxiety and Pelvic Floor Tightness
Muscle tension does not occur in isolation. The pelvic floor functions within a complex communication network between the brain, spinal cord, and surrounding organs. Emotional stress travels along this network in ways that many people underestimate.
Heightened anxiety stimulates the sympathetic branch of the autonomic nervous system. This response evolved as a survival mechanism that primes the body for rapid action. Heart rate increases, breathing becomes shallow, and muscles brace for movement. The pelvic floor participates in this response because it supports core stabilization and protective reflexes.
Chronic activation keeps muscles guarded long after the stressor disappears. When this occurs repeatedly, the pelvic floor gradually adapts to a shortened resting state. The tissue remains strong but loses flexibility and responsiveness. Pelvic physiotherapists frequently observe this pattern in individuals dealing with persistent stress or unresolved anxiety.
A calmer mental state signals the parasympathetic system to take control. Blood flow increases, muscle fibers lengthen, and internal organs function more comfortably. This neurological shift forms the biological foundation behind anxiety reduction strategies for pelvic floor relief.
How the Stress Response Alters Pelvic Floor Muscle Tone
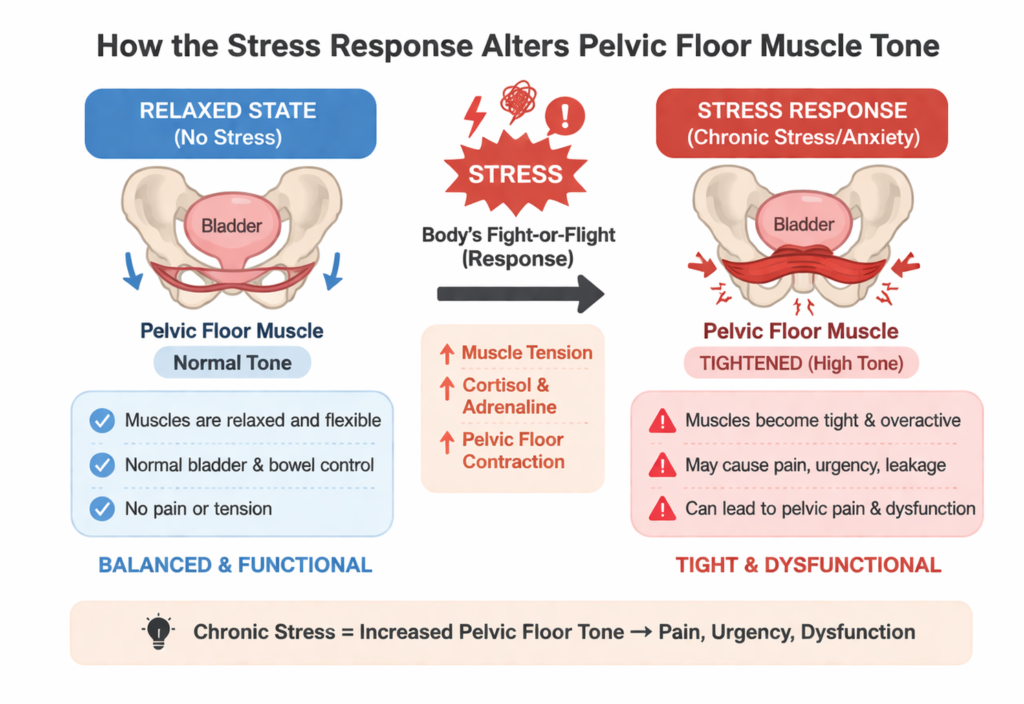
Stress influences the body in layered ways. Pelvic muscles respond not only to mechanical load but also to emotional signals processed by the brain. Even subtle psychological tension can produce physical guarding.
During moments of anxiety, breathing often becomes shallow and chest driven. The diaphragm stops moving through its full range. The pelvic floor works in harmony with the diaphragm during each breath. When breathing remains restricted, pelvic muscles lose their natural rhythm and remain partially contracted.
A prolonged stress response also heightens sensitivity within pelvic nerves. Small sensations that once passed unnoticed begin to feel uncomfortable or painful. Tight muscles compress surrounding nerves and blood vessels, intensifying this feedback loop.
Therapeutic approaches that quiet the nervous system often restore the breathing pattern first. As the diaphragm resumes deeper movement, the pelvic floor begins to synchronize again. This coordination gradually reduces excessive tension.
The Brain-Pelvis Communication Pathway
Neuroscientists describe the pelvic region as highly responsive to emotional states. Several brain areas responsible for threat perception also influence pelvic muscle activity. Signals travel through the spinal cord to activate or relax muscles based on perceived safety.
The brain cannot easily distinguish between physical danger and emotional stress. Work pressure, social worries, or internalized tension may trigger the same muscular reaction as physical threat. Pelvic muscles brace instinctively.
Therapeutic relaxation practices help retrain this communication pathway. When the brain experiences repeated signals of safety, the pelvic floor receives permission to release. Over time, muscle tone becomes more adaptable rather than rigidly guarded.
Why Chronic Anxiety Can Lead to Hypertonic Pelvic Floor Dysfunction
Pelvic physiotherapists often encounter patients who unknowingly hold tension deep in their bodies. Many describe a constant need to clench the abdomen or brace their hips during stressful moments. The pelvic floor becomes part of this habitual pattern.
A Hypertonic Pelvic Floor develops when muscles remain contracted longer than their natural cycle allows. Unlike weakness, which involves reduced strength, hypertonicity involves excessive tension and shortened muscle fibers.
Individuals experiencing this pattern may notice pelvic pain, urinary urgency, constipation, or discomfort during intimacy. These symptoms can feel confusing since the muscles themselves are not injured. They simply lack the ability to lengthen fully.
Chronic anxiety accelerates this pattern. Repeated stress keeps the body in a state of vigilance. The pelvic floor adapts by tightening as a protective reflex, similar to how shoulders tense during pressure. When anxiety persists for months or years, the pelvic floor begins to interpret tension as its default state.
Muscle Guarding and Emotional Stress
Guarding describes the subconscious tightening of muscles to protect vulnerable areas. Many people experience guarding in the jaw, shoulders, or lower back. The pelvic floor responds in the same way, although it remains less visible.
Emotional stress encourages subtle clenching in the lower abdomen and pelvic region. Some individuals hold tension while sitting at a desk. Others clench during intense concentration or emotional strain.
This repeated contraction prevents full relaxation between movements. Over time the muscles shorten and lose elasticity. Pelvic floor therapy frequently focuses on restoring the ability to release rather than strengthening muscles further.
Reducing anxiety removes the constant signal that encourages guarding. Once the brain stops anticipating threat, the pelvic floor gradually releases its defensive posture.
Breathing Patterns and Pelvic Muscle Pressure
Breathing influences internal pressure within the abdomen and pelvis. During relaxed breathing, the diaphragm moves downward while the pelvic floor gently lengthens. During exhalation the pelvic floor recoils upward.
Anxiety disrupts this rhythm. Chest breathing limits diaphragmatic motion and increases pressure in the upper body. The pelvic floor responds by tightening to stabilize the core.
Therapists often notice that individuals with Hypertonic Pelvic Floor symptoms demonstrate restricted breathing patterns. Encouraging slow diaphragmatic breathing restores the natural relationship between the diaphragm and pelvic muscles.
Calmer breathing reduces the internal pressure that maintains pelvic tension. Over time the muscles regain their ability to relax during inhalation.
Psychological Stress and the Pelvic Pain Cycle
Pain rarely exists as a purely physical sensation. The brain interprets pain through emotional and psychological filters. Stress amplifies these signals and increases sensitivity throughout the nervous system.
People experiencing pelvic tension frequently develop anxiety about the symptoms themselves. Worry about discomfort during sitting, urination, or intimacy creates additional stress. This emotional response reinforces muscular guarding.
The body then enters a feedback cycle. Pain increases anxiety, anxiety tightens muscles, and tighter muscles intensify pain. Breaking this cycle requires addressing both the physical and psychological components.
Relaxation techniques calm the nervous system and reduce fear signals sent to pelvic muscles. As anxiety decreases, muscle tone softens and pain sensitivity often diminishes.
How Anxiety Heightens Pain Perception
The brain contains networks that evaluate sensory information before labeling it as pain. Stress hormones influence these networks and make them more reactive.
When anxiety remains elevated, the brain becomes vigilant toward bodily sensations. Small signals from pelvic muscles may feel magnified. This heightened perception encourages protective muscle tightening.
Calming the nervous system reduces this amplification effect. The brain becomes less reactive to minor sensations. Pelvic muscles can relax without constant monitoring from the nervous system.
Emotional Regulation and Muscle Release
Emotions affect muscle tone throughout the body. Fear and worry trigger contraction, while calm emotional states allow muscles to soften.
Practices that support emotional regulation often produce noticeable physical changes. Slow breathing, mindfulness, and body awareness techniques teach the brain to interpret sensations without alarm.
The pelvic floor responds to these shifts with gradual relaxation. Patients working with pelvic health specialists frequently report reduced tightness when anxiety management becomes part of their treatment plan.
Practical Strategies That Calm Anxiety and Relax the Pelvic Floor
Grounding practices reconnect attention to the present moment. They interrupt cycles of worry that stimulate the stress response. As mental focus settles, breathing slows and muscles release.
Body awareness exercises also play an important role. Many individuals are unaware of how often they clench their pelvic muscles throughout the day. Mindful attention helps retrain the body to recognize and release tension patterns.
One technique that therapists frequently recommend involves the 5-4-3-2-1 Grounding exercise. This practice guides attention through sensory awareness and reduces anxious thought loops. As the nervous system quiets, pelvic muscles often respond by relaxing.
The Role of the 5-4-3-2-1 Grounding Method in Muscle Relaxation
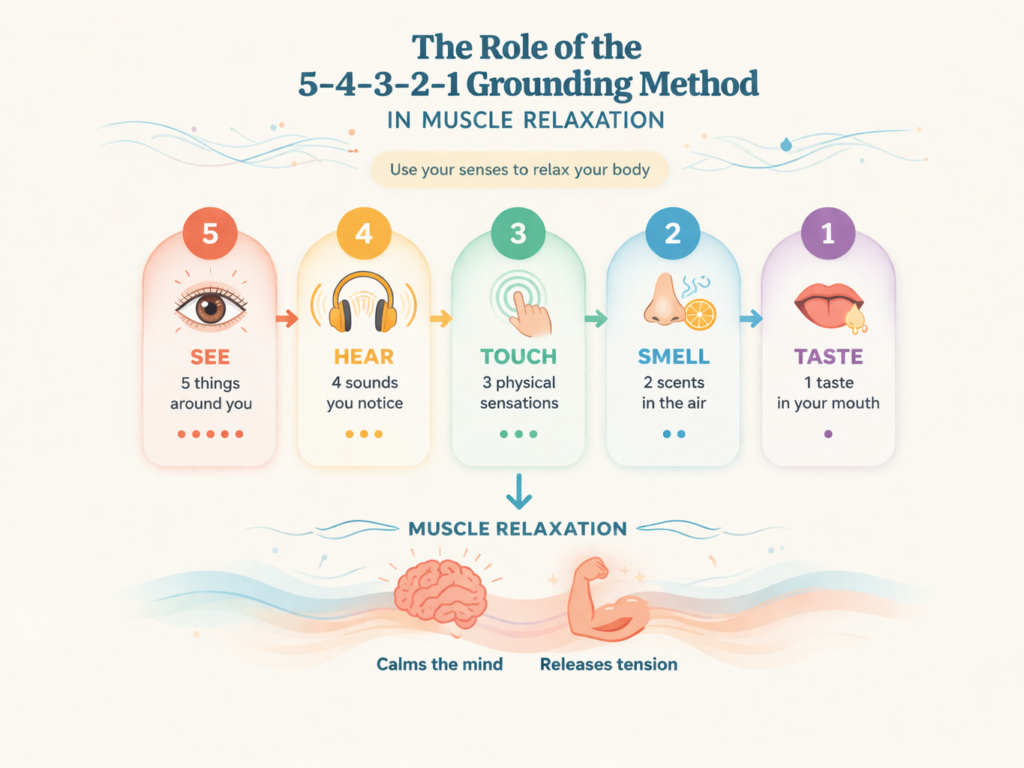
The 5-4-3-2-1 Grounding technique shifts attention away from internal worry and toward external sensory cues. The brain begins focusing on what is seen, touched, heard, smelled, and tasted in the immediate environment.
This sensory orientation interrupts the stress response cycle. Heart rate slows and breathing becomes deeper. Muscles throughout the body soften as the brain recognizes a safe environment.
Pelvic physiotherapists often integrate this practice into relaxation routines. When anxiety settles, the pelvic floor releases subtle tension that previously went unnoticed.
Repeating the 5-4-3-2-1 Grounding method regularly conditions the nervous system to recover from stress more quickly. Over time, pelvic muscles spend less time in a guarded state.
Integrating Breathwork With Pelvic Floor Awareness
Breathwork provides a bridge between mental calm and physical relaxation. Slow diaphragmatic breathing activates the parasympathetic nervous system, the branch responsible for rest and recovery.
As inhalation deepens, the diaphragm descends and the pelvic floor gently lengthens. Exhalation allows the muscles to recoil upward without force. This rhythmic motion restores mobility within the pelvic region.
Combining breathwork with grounding practices strengthens the relaxation response. Anxiety gradually loses its hold on muscle tone.
With consistent practice, individuals often regain the ability to relax pelvic muscles voluntarily. This shift supports recovery from persistent tension patterns.
Clinical Observations From Pelvic Health Specialists
Pelvic health clinicians frequently encounter patients whose symptoms fluctuate with stress levels. Days filled with emotional pressure often coincide with increased pelvic discomfort. Periods of relaxation tend to reduce symptoms noticeably.
Therapists emphasize that muscle tension does not always originate from weakness or injury. The nervous system plays a significant role in regulating pelvic tone. Addressing anxiety therefore becomes part of many treatment plans.
Clinical experience also shows that individuals who learn relaxation techniques early often recover more quickly from pelvic tension. Nervous system regulation allows physical therapies to work more effectively.
These observations highlight the interconnected nature of emotional and physical health. The pelvic floor responds dynamically to changes in mental state.
Behavioral Patterns That Reinforce Pelvic Tightness
Daily habits influence pelvic muscle tone more than many people realize. Long hours of sitting, frequent abdominal bracing, and shallow breathing contribute to ongoing tension.
Stressful work environments encourage unconscious clenching of the lower abdomen and hips. Over time this pattern spreads to the pelvic floor.
Clinicians encourage patients to pause periodically during the day and notice their breathing and muscle tension. Gentle awareness interrupts automatic clenching.
These small behavioral shifts complement therapeutic exercises and support long term pelvic relaxation.
Restoring Muscle Flexibility Through Nervous System Regulation
Muscle fibers regain flexibility when the nervous system allows them to lengthen. Treatments that calm anxiety create favorable conditions for this process.
Pelvic floor therapy often combines manual techniques with breathing exercises and relaxation training. Each component supports the others.
When anxiety decreases, the pelvic floor becomes more responsive to physical therapy. Muscles that once resisted stretching gradually regain mobility and comfort.
Physiological Effects of Anxiety Reduction on Pelvic Function
The body undergoes measurable physiological changes during relaxation. These changes extend directly to pelvic structures and influence muscle tone.
Blood flow increases as stress hormones decline. Improved circulation nourishes muscle tissue and reduces inflammatory signals. Pelvic organs function more smoothly within this environment.
The digestive and urinary systems also benefit from parasympathetic activation. Many pelvic symptoms involve these systems, which share nerve pathways with pelvic muscles.
The following table illustrates how anxiety levels influence pelvic function.
| Anxiety Level | Nervous System State | Pelvic Muscle Response | Physical Sensation | Functional Outcome |
| High stress | Sympathetic activation | Persistent contraction | Pressure and discomfort | Restricted muscle movement |
| Moderate stress | Mixed nervous activity | Partial tension | Mild tightness | Limited relaxation ability |
| Reduced anxiety | Parasympathetic engagement | Gradual muscle release | Warmth and ease | Improved flexibility |
| Calm state | Restorative nervous system | Balanced tone | Comfort and mobility | Healthy pelvic function |
| Sustained calm | Nervous system resilience | Responsive muscle tone | Stable relaxation | Long term pelvic health |
This physiological shift explains why calming anxiety often produces noticeable improvements in pelvic comfort. Muscles function best when the nervous system supports relaxation rather than constant vigilance.
Frequently Asked Questions
Can anxiety alone cause pelvic floor tightness?
Yes. Anxiety activates the body’s stress response, which increases muscle tension throughout the body. The pelvic floor participates in this protective reaction. Chronic anxiety can lead to persistent contraction patterns associated with Hypertonic Pelvic Floor symptoms.
How quickly can anxiety reduction affect pelvic floor tension?
Changes sometimes appear within minutes during relaxation exercises. Long standing tension patterns usually require repeated nervous system regulation over weeks or months. Consistency plays a major role in restoring balanced muscle tone.
Does the 5-4-3-2-1 grounding technique directly relax pelvic muscles?
The 5-4-3-2-1 Grounding exercise reduces mental stress and activates calming neural pathways. When the brain shifts into a safer state, muscles throughout the body respond by releasing tension, including those within the pelvic floor.
Is pelvic floor strengthening helpful for tight muscles?
Strengthening alone may worsen symptoms when muscles are already excessively tight. Pelvic therapists usually focus on relaxation, breathing coordination, and gentle mobility exercises when treating Hypertonic Pelvic Floor conditions.
Why does pelvic pain worsen during stressful periods?
Stress hormones increase nerve sensitivity and muscle guarding. Pelvic muscles may tighten unconsciously during anxious moments, intensifying discomfort or pressure sensations.
Can grounding exercises be combined with pelvic floor therapy?
Yes. Techniques such as the 5-4-3-2-1 Grounding practice often complement physical therapy. Calming the nervous system allows manual treatments and breathing exercises to work more effectively.
Closing Perspective
Pelvic floor tension rarely exists as an isolated muscular issue. The nervous system constantly monitors emotional signals and adjusts muscle tone in response. Anxiety encourages protective contraction, while calm mental states permit muscles to lengthen and function naturally.
Relief often begins when attention shifts from forcing muscles to relax toward calming the nervous system itself. Practices that reduce anxiety gradually retrain the body to release habitual tension patterns. As this shift unfolds, the pelvic floor regains its natural rhythm of contraction and relaxation, restoring comfort and mobility throughout the pelvic region.
Health
How Cocaine Cut With Levamisole Can Trigger Shocking Skin Necrosis

Cocaine already carries serious risks, but the danger becomes even harder to read when the drug is mixed with something most users never see, smell, or ask for. One of the most alarming examples is levamisole, a drug once used in human medicine and also known as an anti-parasitic agent. When it shows up in cocaine, it can do something that sounds almost unreal: it can help trigger blood vessel damage, purple rashes, and areas of dead skin. Medical reports have linked levamisole-adulterated cocaine with vasculitis, retiform purpura, and skin necrosis, often affecting the ears, face, and limbs.
And here’s the thing. This kind of damage does not always start as a dramatic wound. Sometimes it begins as a bruise-like patch, a painful rash, or a strange purple mark on the ear. Then it changes. The skin darkens. The pain grows sharper. Tissue starts to break down. What looks like a skin problem is really a warning sign from the blood vessels underneath.
The Cut You Don’t See Coming
Levamisole is not added to cocaine because it helps the body. It is an adulterant, meaning it is mixed into the drug supply before it reaches the user. For the person taking cocaine, there is usually no obvious clue that levamisole is there. The powder does not come with a label. There is no neat ingredient list. No red flag on the bag.
That uncertainty is part of what makes this issue so disturbing. A person may think they are dealing with the usual risks of cocaine, but the body is actually facing a second chemical insult. Levamisole has been associated with immune system disruption and abnormal antibody responses. In plain terms, the immune system can become confused and begin attacking small blood vessels.
Why the Skin Shows the Damage First
Skin is often where the story becomes visible. Blood vessels feed the skin with oxygen and nutrients. When those small vessels become inflamed, blocked, or damaged, the skin above them suffers.
That is why the rash can look patchy, dark, or web-like. Doctors often call this retiform purpura, a pattern that can resemble branching lines or irregular purple islands. It is not just “a rash.” It is a sign that blood flow has gone wrong.
The ears are a strange but classic site. Medical case reports have described purplish lesions and necrosis on the ear lobes and rims, along with similar changes on the thighs, legs, and other extremities.
When a Rash Isn’t Just a Rash
Most people have had a rash at some point. Heat rash. Allergy rash. A weird patch after using a new soap. So it’s easy to understand why someone might first dismiss early skin changes. Honestly, that’s what makes this so dangerous.
Levamisole-linked skin injury can look like bruising, purple blotches, blisters, or blackened patches. It can also hurt. Sometimes the affected areas feel tender before they look severe. In other cases, the skin changes fast enough to feel frightening, like the body has skipped a few warning steps.
This is where the word “necrosis” matters. Necrosis means tissue death. Not irritation. Not dryness. Death of skin tissue. Once skin dies, the body cannot simply smooth it back into place like a scraped knee. The area can become an open wound. Infection can follow. Scarring can remain.
A recovery center for addiction can become part of the wider conversation when cocaine use keeps placing a person back in contact with a contaminated drug supply. The skin injury is only one visible part of a larger pattern, and the visible part can be brutal.
The Immune System Gets Pulled Into the Mess
The immune system is meant to protect you. With levamisole-adulterated cocaine, it can become part of the damage. Researchers have noted that many patients with this condition show abnormal immune markers, including ANCA antibodies, which are often linked with blood vessel inflammation.
Think of it like a security alarm that starts attacking the building it was meant to guard. The body reacts, but the reaction turns messy. Small vessels become inflamed. Clots can form. Blood cannot move through certain areas as it should. Then the skin pays the price.
It is ugly chemistry, but it is also very human. Because nobody using cocaine casually at a party, after work, or during a weekend binge is thinking about antibody patterns and small-vessel vasculitis. They are thinking about the moment. The body, though, keeps the receipt.
Why the Ears and Extremities Are So Often Mentioned
The ears tend to catch attention in these cases because they are visible and unusual. A purple, painful ear does not fit the mental picture most people have of drug-related harm. People expect nosebleeds, chest pain, anxiety, or weight loss. They do not expect the rim of the ear to turn dark.
But the ears and extremities have delicate blood supply patterns. When blood vessels tighten, inflame, or clot, these areas can show damage quickly. Fingers, toes, legs, cheeks, and ears can all become part of the same disturbing map.
Medical literature has described frequent involvement of the ear lobes, the skin over the cheekbone area, and the lower extremities, with less involvement of the trunk and back. Purpuric plaques and central necrosis have also been reported in a notable share of cases.
There is something especially unsettling about skin damage in visible places. It makes private drug exposure public. A person may be able to hide use for months or years, then suddenly the skin tells the story first. Not gently, either.
Contaminated Cocaine Changes the Risk Picture
The street drug supply is not stable. It shifts by region, batch, dealer, and demand. Cocaine contamination adds another layer of risk because the person using it often does not know what they are taking. That means the danger is not only cocaine itself, but also the unknown mixture riding along with it.
Levamisole became a major concern because it was repeatedly found in seized cocaine in North America and Europe, and doctors began linking it with distinctive cases of purpura, vasculitis, neutropenia, and necrosis.
Neutropenia is another important word here. It means the body has a low count of neutrophils, a type of white blood cell that helps fight infection. So the same contamination linked with skin wounds can also weaken the body’s defence system. That is a rough combination: damaged skin plus reduced infection-fighting power.
You know what? That is the part that often gets missed in public talk about drugs. The conversation tends to stay moral, dramatic, or criminal. But the body does not care about slogans. It reacts to chemicals, blood flow, immune signals, tissue damage, and infection risk.
The Skin Can Become a Medical Crime Scene
A necrotic patch of skin is not just a surface wound. It is evidence of something deeper happening underneath. Doctors often look at the pattern, the location, the person’s drug exposure, blood tests, and sometimes a biopsy. In reported cases, biopsies have shown small-vessel vasculitis, clotting, inflammation, and blood leaking into the skin.
That is why these wounds can feel so out of proportion. A person may think, “How did a rash become this?” The answer is that it was never only a rash. It was a vascular event showing through the skin.
There is also a social layer. People with substance use problems often delay care because of shame, fear, cost, or bad past treatment by the system. Skin wounds then worsen in silence. A small purple area becomes a black patch. A black patch becomes an open wound. And by then, the problem has moved from scary to serious.
A phrase like Therapy For Addiction Recovery belongs in this wider discussion because cocaine-related harm is rarely just about one bad batch. It often sits inside stress, compulsive use, mental health strain, and repeated exposure to risk. The skin can show the crisis, but it does not explain the whole life behind it.
Why This Story Feels So Shocking
Part of the shock comes from contrast. Cocaine is often portrayed through nightlife, money, work pressure, celebrity culture, or quiet middle-class use. Levamisole-linked necrosis cuts through that image. It is not glossy. It is not glamorous. It is skin turning purple, black, and painful because tiny blood vessels are under attack.
There is also the betrayal factor. People know illegal drugs are risky, yes. But contamination feels different. It means the user is not only gambling with cocaine’s known effects. They are also gambling with hidden additives. The body becomes the testing ground.
And the skin makes it impossible to look away. Skin is identity. It is how people face the world. When necrosis affects the ears, cheeks, legs, or hands, the damage is not abstract. It is visible in the mirror. It can change how someone moves through work, relationships, and ordinary errands. Even a trip to the shop can feel loaded when the body carries a mark people notice.
The Bigger Warning Written on the Skin
Levamisole-adulterated cocaine shows how contaminated drug supplies can turn a private act into a visible medical emergency. The skin becomes the first billboard. Purple rash. Pain. Blisters. Black tissue. A strange mark on the ear that should not be ignored.
But the bigger story is not only about skin. It is about how unpredictable cocaine becomes when adulterants enter the supply. It is about immune reactions that spiral in the wrong direction. It is about delayed care, fear, stigma, and the way a hidden chemical can leave a very public wound.
The most chilling part is simple: the person using the drug usually does not know levamisole is there. They only see what happens after the body starts responding. And by then, the warning is already written on the skin.
Health
How Online Weight Loss Prescriptions Work

More than 1.6 million people in the UK took advantage of weight-loss drugs last year, and online prescriptions for these products work by connecting patients with licensed clinicians through secure digital platforms to facilitate medical screenings and ongoing treatment. This model replaces traditional in-person waiting rooms with asynchronous consultations or video calls, streamlining care for metabolic health.
The Digital Path To Medical Weight Management
There are thousands of patients seeking obesity treatment every day who find the traditional clinical route inaccessible or intimidating. The process typically begins with an eligibility screening where you provide your medical history, current BMI, and any pre-existing conditions. If you meet the clinical criteria, a prescriber reviews your file to determine if a GLP-1 medication is appropriate for your specific health profile.
Safety is the cornerstone of this process, particularly when dealing with potent medications like Tirzepatide weight management care which requires careful oversight. Available in the US via online outlets, Brits have other considerations to keep in mind.
Specifically, UK providers must adhere to GPhC prescribing requirements, which mandate independent verification of a patient’s identity and health metrics. This ensures that the person receiving the medication is the same person who underwent the clinical evaluation.
Once a prescription is issued, it is sent electronically to a registered pharmacy. The medication is then shipped in temperature-controlled packaging to maintain the integrity of the peptides.
Eligibility And Safety Protocols For GLP-1 Therapy
Navigating the world of online prescriptions requires an understanding of what makes a provider trustworthy. In the UK, a legitimate service will always check your BMI against specific thresholds and ask for a summary of your recent blood tests or GP records. They prioritise patient safety over quick sales, often screening out those with contraindications like a family history of medullary thyroid cancer.
Clinical data suggest that the delivery of these drugs is only half of the equation. Maximally engaged users on tirzepatide achieve significantly higher weight loss percentages when they utilise digital behavioural support tools alongside their medication. This holistic approach prevents the “rebound effect” often seen when medication is used in a vacuum without lifestyle modifications.
Legitimate platforms follow a specific sequence of operations to ensure patient care remains the priority:
- Patients complete a comprehensive health questionnaire covering metabolic and mental health
- A clinician reviews the data and may request additional evidence, such as photos or GP letters
- The pharmacy fulfils the order only after a digital signature is captured from the prescriber
This structured workflow protects the patient and ensures the clinician has all the necessary data points to make an informed decision. If a site offers medication without a consultation or skips the medical history phase, it is a significant red flag for an unsafe provider.
Privacy And Professional Standards In Telehealth
Privacy is a major driver for the shift toward online prescribing. Many individuals feel a sense of stigma when discussing weight management in a crowded GP surgery. Digital platforms use encrypted e-consent forms and secure messaging portals to protect sensitive health data in compliance with strict GDPR and healthcare privacy laws.
The rise of these services has also helped bridge the gap created by NHS rollout constraints, which often limit access to only the most severe cases. Private telehealth providers allow individuals who may not meet the extremely high BMI requirements of the NHS to access the same high-quality, regulated medications.
You are not just buying a product; you are entering a clinical relationship. This relationship includes regular check-ins to monitor side effects and adjust dosages as you move through the titration schedule. The goal is to move you toward a healthier metabolic state while ensuring the medication remains effective and well-tolerated over the long term, alongside other wellness efforts such as minimising anxiety for pelvic floor benefits and eating nutritious food.
Navigating Modern Weight Care Safely
Choosing a provider is the most critical step in your journey. Always look for the green GPhC registration badge on the website and verify that the clinicians are registered with the General Medical Council. By following a regulated path, you ensure that the medication you receive is authentic, safe, and part of a comprehensive plan for your future health.
The depth of support provided by top-tier platforms often includes access to nutritionists and fitness coaches who understand the nuances of GLP-1 therapy. This multi-pronged approach is what separates a simple prescription service from a true medical weight management program. To learn more about managing modern life’s ups and downs, read our other posts.
Health
Stem Cell Therapy: Conditions and Medical Indications Explained
Stem cell therapy has emerged as one of the most promising advancements in modern medicine. It is widely used in the treatment of various complex and chronic diseases where traditional therapies may have limited success. Understanding the conditions and indications for stem cell therapy is essential for determining when this innovative treatment can be applied effectively.
Leading healthcare institutions such as Liv Hospital are at the forefront of stem cell research and clinical applications, offering advanced treatment options for eligible patients.
What Are Stem Cell Conditions and Indications?
Stem cell conditions and indications refer to the specific diseases and medical situations in which stem cell therapy may be recommended. These are carefully evaluated by specialists based on the patient’s overall health, disease severity, and treatment history.
You can explore more detailed medical information here Stem Cell Conditions and Indications
Role of Stem Cell Therapy in Modern Medicine
Stem cells have the ability to regenerate damaged tissues and support the body’s natural healing process. Because of this, they are used in a variety of medical fields including hematology, oncology, immunology, and regenerative medicine.
Advanced care and treatment services are available at Liv Hospital
Common Conditions Treated with Stem Cell Therapy
Stem cell therapy is not suitable for every condition, but it is widely used in several serious medical cases.
1. Blood Disorders
- Leukemia
- Lymphoma
- Aplastic anemia
- Multiple myeloma
2. Bone Marrow Diseases
- Bone marrow failure
- Myelodysplastic syndromes
3. Autoimmune Diseases
- Multiple sclerosis
- Systemic lupus erythematosus
- Rheumatoid arthritis
4. Neurological Conditions
- Spinal cord injuries
- Parkinson’s disease
- Neurodegenerative disorders
5. Metabolic and Genetic Disorders
- Certain inherited blood and immune system diseases
When Is Stem Cell Therapy Recommended?
Doctors consider stem cell therapy when:
- Standard treatments are not effective
- The disease is progressive or life-threatening
- Bone marrow or blood production is severely affected
- The patient is medically fit for transplantation
Each case is carefully evaluated to ensure safety and effectiveness.
Importance of Proper Medical Evaluation
Before starting stem cell therapy, a detailed evaluation is necessary. This includes:
- Blood tests
- Bone marrow examination
- Genetic testing
- Overall health assessment
This ensures that only suitable patients receive treatment, improving success rates and reducing risks.
Why Choose Advanced Medical Centers?
Successful stem cell therapy depends heavily on the expertise of the medical center. Institutions like Liv Hospital provide:
- Specialized stem cell units
- Advanced diagnostic technology
- Experienced multidisciplinary teams
- International treatment standards
- Personalized patient care
Conclusion
Stem cell therapy offers new hope for patients with complex and difficult-to-treat conditions. Understanding the conditions and indications for stem cell therapy is essential for safe and effective treatment planning. With world-class medical institutions like Liv Hospital, patients can access advanced regenerative treatments supported by expert care and modern medical technology.
-

 Celebrity6 months ago
Celebrity6 months agoNancy Hallam: The Inspiring Life, Career, and Success Story Behind Ian Wright’s Wife
-

 Celebrity7 months ago
Celebrity7 months agoJohnny Carell: Inside the Life, Family, and Rising Success of Steve Carell’s Son
-

 Celebrity6 months ago
Celebrity6 months agoWho Is Maisie Mae Roffey? The Private Life, Family Story, and Quiet Success of Julie Walters’ Daughter
-

 Health4 months ago
Health4 months agoEnclomimed 25 (Enclomiphene) – Effective PCT Protocol
-

 Celebrity5 months ago
Celebrity5 months agoWho Is Cameron Kade Hickenbottom? Shawn Michaels’ Son and His Independent Creative Legacy
-

 Business5 months ago
Business5 months agoSimon Dixon Biography: Lifestyle, Net Worth, Family, Career and Success Story
-

 Celebrity4 months ago
Celebrity4 months agoWho Is Mark Gero? Inside the Life, Art, and Quiet Legacy of an American Creative
-

 Celebrity4 months ago
Celebrity4 months agoDraven Duncan: Tim Duncan’s Rising Star Son and His Inspiring Basketball Journey






